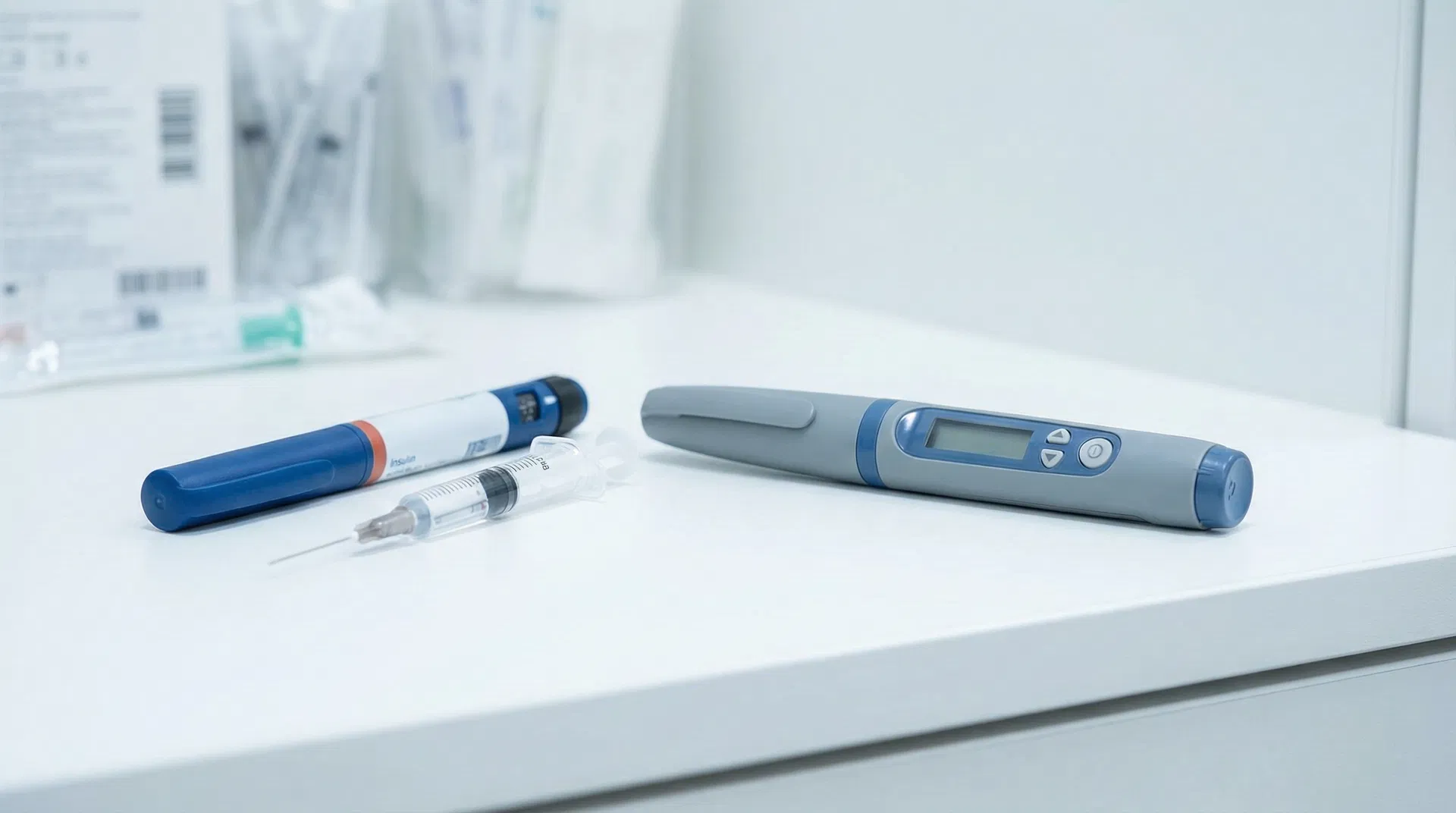
Insulin vs. GLP-1 Agonists: Which Is Better for Type 2 Diabetes?
For decades, insulin was the go-to injectable medication for patients with type 2 diabetes whose blood sugar could not be controlled with oral medications. Today, GLP-1 receptor agonists like Ozempic (semaglutide), Trulicity (dulaglutide), and Mounjaro (tirzepatide) have emerged as powerful alternatives that, for many patients, offer better outcomes with fewer risks.
This guide explains the fundamental differences between insulin and GLP-1 agonists, when each is the right choice, and why the treatment landscape for type 2 diabetes has shifted dramatically over the past decade.
The Fundamental Difference: Replacing vs. Stimulating
The most important distinction between insulin and GLP-1 agonists is what they do to the body's own hormone systems.
Insulin is a hormone replacement therapy. In type 2 diabetes, the pancreas still produces insulin but either not enough of it or the body's cells have become resistant to its effects. Injecting insulin directly supplies the hormone the body needs to move glucose from the bloodstream into cells. It is a direct, powerful intervention that works regardless of how much residual pancreatic function remains.
GLP-1 agonists work by stimulating the body's own insulin-producing system. They mimic the gut hormone GLP-1, which signals the pancreas to release insulin in response to rising blood sugar. Crucially, this stimulation is glucose-dependent — GLP-1 agonists only trigger insulin release when blood sugar is actually elevated. When blood sugar is normal or low, the GLP-1 signal is weak, which is why these drugs carry a much lower risk of hypoglycemia than insulin.
This distinction has profound clinical implications. GLP-1 agonists require a functioning pancreas to work — they are ineffective in type 1 diabetes and in late-stage type 2 diabetes where beta cell function is severely depleted. Insulin, by contrast, works regardless of pancreatic function.
Head-to-Head Comparison
| Feature | Insulin (Basal) | GLP-1 Agonists |
|---|---|---|
| Mechanism | Replaces deficient insulin | Stimulates endogenous insulin release |
| A1c reduction | 1.5–2.5% | 1.0–2.0% |
| Weight effect | Weight gain (2–4 kg) | Weight loss (3–6 kg) |
| Hypoglycemia risk | Moderate to high | Very low |
| Cardiovascular benefit | Neutral | Strong (liraglutide, semaglutide, dulaglutide) |
| Requires functioning beta cells | No | Yes |
| Injection frequency | Daily (basal) | Weekly (most agents) |
| Dose titration complexity | High | Low to moderate |
| Monthly cost (no insurance) | $25–$300 (human insulin) to $300–$500 (analogs) | $800–$1,000 |
| Generic/biosimilar available | Yes (human insulin, some analogs) | No |
Weight: The Critical Difference
One of the most clinically significant differences between insulin and GLP-1 agonists is their effect on body weight — and the effects point in opposite directions.
Insulin causes weight gain. This is not a side effect that can be avoided with careful dosing — it is a direct consequence of insulin's mechanism. Insulin promotes fat storage and prevents fat breakdown. Patients starting insulin therapy typically gain 2–4 kg in the first year, and weight gain can be substantially more with intensive insulin regimens. For patients with type 2 diabetes who are already overweight or obese, this weight gain worsens insulin resistance and can create a cycle where more insulin is needed to achieve the same blood sugar control.
GLP-1 agonists cause weight loss. By acting on appetite centers in the brain and slowing gastric emptying, GLP-1 agonists reduce food intake and promote weight loss. At standard diabetes doses, patients typically lose 3–6 kg. At higher doses used specifically for obesity (such as Wegovy, the weight loss formulation of semaglutide), weight loss of 10–15% of body weight is achievable. This weight loss improves insulin sensitivity and can actually reduce the amount of diabetes medication needed over time.
For patients with significant obesity, this difference alone is often decisive.
Hypoglycemia Risk
Hypoglycemia — dangerously low blood sugar — is one of the most serious risks of insulin therapy. Because insulin lowers blood sugar regardless of the current glucose level, a dose that is too high, a missed meal, or unexpected exercise can drive blood sugar below safe levels. Severe hypoglycemia can cause seizures, loss of consciousness, and in rare cases, death.
GLP-1 agonists have a fundamentally different risk profile. Because their insulin-stimulating effect is glucose-dependent, they do not cause hypoglycemia when used as monotherapy or in combination with metformin. The risk of hypoglycemia increases when GLP-1 agonists are combined with insulin or sulfonylureas, but even then the risk is lower than with insulin alone.
For elderly patients, patients who live alone, patients who drive professionally, or patients with hypoglycemia unawareness, the lower hypoglycemia risk of GLP-1 agonists is a major clinical advantage.
Cardiovascular Outcomes
The cardiovascular benefit data strongly favors GLP-1 agonists over insulin.
Multiple large cardiovascular outcomes trials have demonstrated that GLP-1 agonists reduce the risk of major adverse cardiovascular events (heart attack, stroke, cardiovascular death) in patients with type 2 diabetes and established cardiovascular disease or high cardiovascular risk:
- Liraglutide (Victoza): LEADER trial — 13% reduction in MACE
- Semaglutide (Ozempic): SUSTAIN-6 trial — 26% reduction in MACE
- Dulaglutide (Trulicity): REWIND trial — 12% reduction in MACE
Insulin, by contrast, has not demonstrated cardiovascular benefit in large outcomes trials. The ORIGIN trial, which randomized over 12,000 patients with pre-diabetes or early type 2 diabetes to insulin glargine vs. standard care, found no reduction in cardiovascular events.
This cardiovascular benefit data has fundamentally changed treatment guidelines. The 2023 ADA Standards of Care now recommend GLP-1 agonists with proven cardiovascular benefit as preferred agents for patients with established cardiovascular disease, regardless of A1c level.
When Insulin Is Still the Right Choice
Despite the advantages of GLP-1 agonists, there are important clinical situations where insulin remains the preferred or necessary treatment:
Very high A1c (above 10–11%). When blood sugar is severely elevated, the rapid and powerful glucose-lowering effect of insulin may be needed to bring A1c under control quickly. GLP-1 agonists are effective but may not act quickly enough in severe hyperglycemia.
Depleted beta cell function. In patients with long-standing type 2 diabetes where the pancreatic beta cells have been significantly damaged, GLP-1 agonists have limited effectiveness because they rely on stimulating insulin secretion from functioning beta cells. These patients may need insulin regardless of other considerations.
Type 1 diabetes. GLP-1 agonists are not approved for type 1 diabetes and are not effective as primary therapy. Insulin is essential for all patients with type 1 diabetes.
Pregnancy. Insulin is the preferred medication for managing diabetes during pregnancy. GLP-1 agonists are not recommended during pregnancy due to limited safety data.
Cost constraints. Human insulin (NPH and regular) is available over the counter at Walmart for $25 per vial. For patients without insurance who cannot afford GLP-1 agonists, human insulin remains an accessible option.
The Shifting Treatment Paradigm
A decade ago, the standard progression for type 2 diabetes was: start with metformin, add oral agents as needed, and eventually add insulin when oral medications were no longer sufficient. GLP-1 agonists were considered a niche option.
Today, that paradigm has shifted significantly. Current guidelines from the ADA, AACE, and the European Association for the Study of Diabetes (EASD) now recommend:
- For patients with established cardiovascular disease or high cardiovascular risk: add a GLP-1 agonist with proven cardiovascular benefit early in treatment, before considering insulin
- For patients with significant obesity: prefer GLP-1 agonists over insulin due to the weight loss benefit
- For patients with very high A1c or symptomatic hyperglycemia: consider short-term insulin to rapidly lower blood sugar, then transition to GLP-1 agonists once control is achieved
The growing availability of combination GLP-1/insulin products (such as Xultophy, which combines insulin degludec with liraglutide, and Soliqua, which combines insulin glargine with lixisenatide) has also blurred the line between these two approaches, allowing patients to benefit from both mechanisms simultaneously.
Practical Considerations: Injections and Monitoring
Both insulin and GLP-1 agonists require injections, but the experience is quite different.
Insulin typically requires daily injections (basal insulin) or multiple daily injections (basal-bolus regimens). Patients on insulin also need to monitor blood glucose regularly — often multiple times per day — to adjust doses and detect hypoglycemia. Dose titration is ongoing and requires patient engagement and education.
GLP-1 agonists are typically injected once weekly (semaglutide, dulaglutide, exenatide extended-release) or once daily (liraglutide, exenatide). They do not require routine blood glucose monitoring when used without insulin. The dose titration is simpler — most agents start at a low dose for 4 weeks to minimize GI side effects, then increase to the maintenance dose.
For patients who are injection-averse, oral semaglutide (Rybelsus) provides the option of a once-daily pill that delivers the same active ingredient as Ozempic, though with somewhat lower bioavailability and efficacy.
Key Takeaways
The choice between insulin and GLP-1 agonists for type 2 diabetes is no longer straightforward. For many patients — particularly those with cardiovascular disease, obesity, or significant hypoglycemia risk — GLP-1 agonists now offer a better benefit-risk profile than insulin. For patients with very high A1c, depleted beta cell function, or cost constraints, insulin remains an important and effective option.
The most important message is that these are not mutually exclusive choices. Many patients use both, and the combination of a GLP-1 agonist with basal insulin is one of the most effective regimens available for patients with advanced type 2 diabetes.
For a comprehensive overview of all available diabetes medications, see our Type 2 Diabetes Medications Guide.
This article is for informational purposes only and does not constitute medical advice. Always consult your healthcare provider before starting, stopping, or changing any medication.
About the Author
RxGuide Editorial Team, PharmD, RPh
Clinical Pharmacist & Medical Writer
The RxGuide editorial team is composed of licensed pharmacists and clinical medical writers with expertise in pharmacology, drug safety, and patient education. All clinical content is reviewed against current FDA labeling, peer-reviewed literature, and established clinical guidelines before publication.