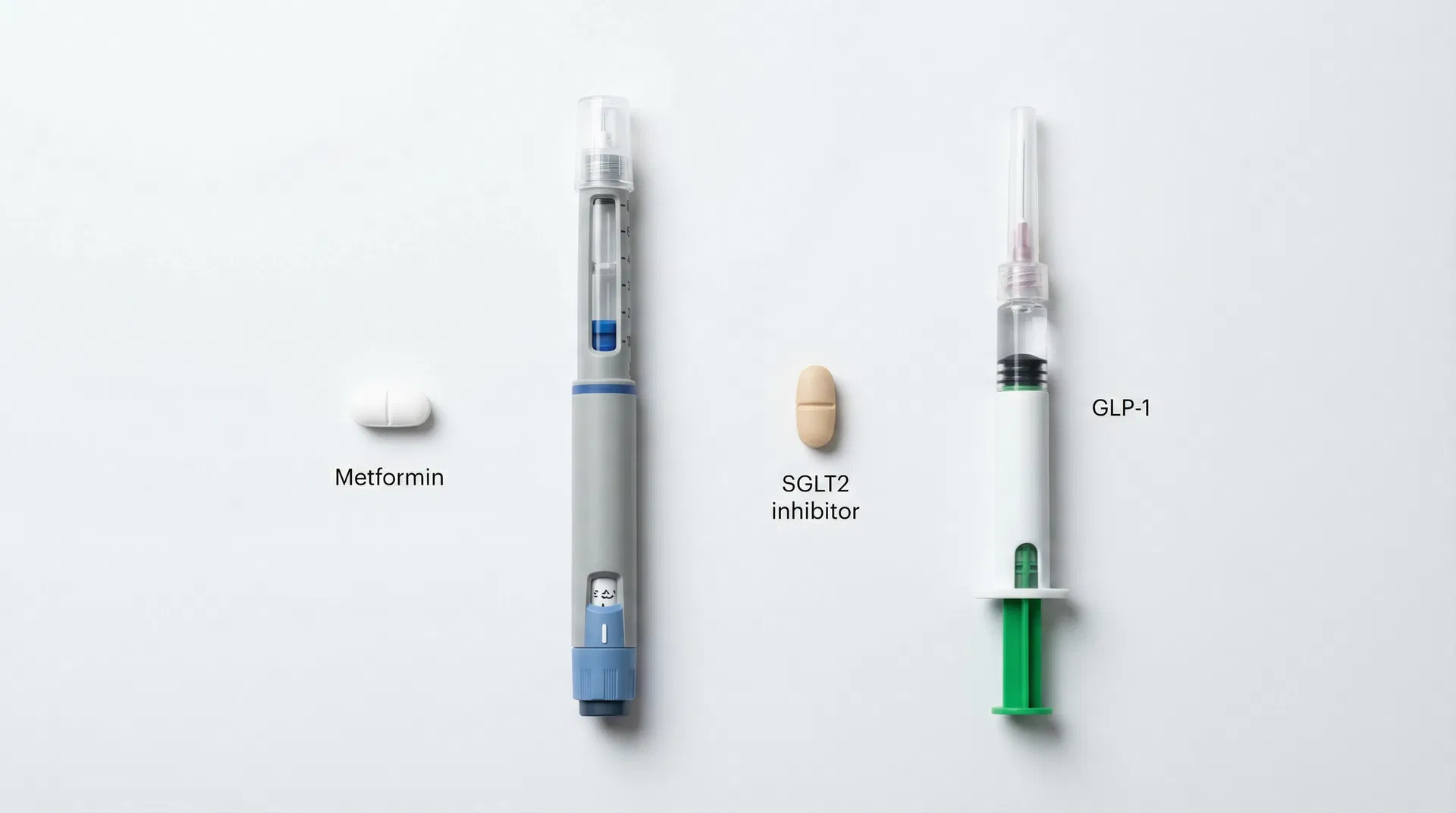
Type 2 Diabetes Medications Explained
This comprehensive guide breaks down the six major classes of Type 2 Diabetes medications, helping you understand how they work, their benefits, and what to expect during treatment.
Key Takeaways
- Metformin remains the gold-standard first-line treatment due to its proven safety, effectiveness, and low cost.
- Newer drug classes like GLP-1 receptor agonists and SGLT2 inhibitors offer significant benefits beyond blood sugar control, including weight loss and heart protection.
- Each medication class works differently—some stimulate insulin production, while others help the body use insulin better or remove excess sugar through urine.
- Choosing the right medication is a personalized process based on your A1C goals, heart health, weight, and potential side effects.
Managing Type 2 Diabetes has evolved significantly over the last decade. While lifestyle changes like diet and exercise remain the foundation of care, most patients will eventually require medication to maintain healthy blood sugar levels. Today, there are more options than ever, ranging from traditional oral pills to advanced weekly injections that also protect the heart and kidneys. Understanding these options is the first step toward a successful treatment plan tailored to your specific health needs.
Understanding the Role of Medication in Type 2 Diabetes
When you have Type 2 Diabetes, your body either doesn't produce enough insulin or cannot use it effectively—a condition known as insulin resistance. The primary goal of Type 2 Diabetes medications is to lower blood glucose (sugar) levels to prevent long-term complications such as nerve damage, kidney disease, and vision loss. Most healthcare providers use the A1C test—a measure of your average blood sugar over three months—to determine if your current treatment is working.
The American Diabetes Association (ADA) typically recommends starting with metformin unless there is a specific reason not to. However, if A1C targets are not met within three to six months, or if a patient has existing heart or kidney disease, additional medications are often added. This "combination therapy" approach allows doctors to target diabetes from multiple angles, such as improving insulin sensitivity while also reducing the amount of sugar the liver produces. It is common for patients to be on two or even three different classes of medication simultaneously to achieve their health goals.
The Biguanide Class: Metformin
The biguanide class currently consists of only one medication: metformin hydrochloride. Despite being decades old, it remains the most widely prescribed diabetes drug in the world. It is favored by clinicians because it is highly effective at lowering A1C, does not cause weight gain, and carries a very low risk of hypoglycemia (dangerously low blood sugar) when used alone.
How Metformin Works
Metformin works primarily by telling the liver to stop overproducing glucose. In people with Type 2 Diabetes, the liver often releases too much sugar into the bloodstream, even when the body doesn't need it. Additionally, metformin improves insulin sensitivity, making it easier for your muscles to take in and use the sugar already in your blood. It also slightly decreases the amount of sugar your intestines absorb from food. By addressing these three different pathways, metformin provides a robust foundation for blood sugar management.
Common Side Effects and Considerations
The most frequent side effects of metformin are gastrointestinal, including nausea, bloating, and diarrhea. These symptoms are usually temporary and can often be minimized by starting with a low dose and taking the medication with a meal. An extended-release (ER) version is also available, which many patients find easier on the stomach. Long-term use of metformin has been linked to Vitamin B12 deficiency, so your doctor may monitor your levels periodically. It is important to note that metformin is generally avoided in patients with advanced kidney disease due to a rare but serious risk of lactic acidosis.
GLP-1 Receptor Agonists: The Incretin Mimics
GLP-1 receptor agonists have revolutionized diabetes care. These medications mimic a natural hormone in your body called glucagon-like peptide-1 (GLP-1). While originally known for blood sugar control, they are now equally famous for their ability to promote significant weight loss and reduce the risk of major cardiovascular events like heart attacks and strokes [1].
Mechanism and Administration
When you eat, your gut releases GLP-1, which signals the pancreas to release insulin in response to the rising sugar. In people with Type 2 Diabetes, this response is often weakened. GLP-1 medications, such as semaglutide (available as Ozempic or Rybelsus), which is often compared in discussions like Ozempic vs Wegovy, restore this signal. They also slow down "gastric emptying," meaning food stays in your stomach longer, making you feel full faster and for a longer duration. Most GLP-1s are administered via a pre-filled injection pen once a week, though a daily oral tablet is also available for those who prefer to avoid needles.
Benefits Beyond Blood Sugar
For patients with established heart disease or chronic kidney disease, GLP-1 agonists are often a preferred second-line choice after metformin. They have been shown to reduce the progression of kidney damage and provide "cardioprotection" by reducing inflammation and improving the health of blood vessels. The weight loss associated with these drugs—often ranging from 5% to 15% of body weight—can also lead to improvements in blood pressure and cholesterol levels, further reducing overall health risks [2].
SGLT2 Inhibitors: The Glucose Flushers
SGLT2 inhibitors represent another modern class of medications that work through a unique mechanism: the kidneys. Unlike most other diabetes drugs that focus on insulin, these medications help the body get rid of excess sugar through urination.
How SGLT2 Inhibitors Function
Normally, your kidneys filter sugar out of the blood and then reabsorb it back into the body. Sodium-glucose cotransporter 2 (SGLT2) is the protein responsible for most of this reabsorption. By blocking this protein, medications like empagliflozin (Jardiance) allow excess sugar to be flushed out in your urine. This process not only lowers blood sugar but also provides a mild diuretic effect, which can help lower blood pressure and reduce swelling.
Heart and Kidney Protection
Clinical trials have demonstrated that SGLT2 inhibitors are exceptionally effective at reducing the risk of hospitalization for heart failure, even in patients who do not have diabetes. They are also highly protective of the kidneys, often slowing the decline of kidney function in patients with diabetic nephropathy [3]. Because they don't rely on insulin to work, they have a very low risk of causing hypoglycemia. However, patients should be aware of the increased risk of genital yeast infections and urinary tract infections due to the higher sugar content in the urine.
| Medication Class | Common Examples | A1C Reduction | Weight Effect | Primary Benefit |
|---|---|---|---|---|
| Biguanides | Metformin | High (1-2%) | Neutral/Loss | First-line, low cost |
| GLP-1 Agonists | Semaglutide, Liraglutide | Very High (1-2%+) | Significant Loss | Heart & Kidney protection |
| SGLT2 Inhibitors | Empagliflozin, Canagliflozin | Intermediate (0.5-1%) | Loss | Heart failure protection |
| DPP-4 Inhibitors | Sitagliptin, Linagliptin | Intermediate (0.5-0.8%) | Neutral | Well-tolerated, oral pill |
| Sulfonylureas | Glipizide, Glimepiride | High (1-2%) | Gain | Fast-acting, inexpensive |
| Thiazolidinediones | Pioglitazone | High (0.5-1.4%) | Gain | Improves insulin sensitivity |
DPP-4 Inhibitors: The Gentle Regulators
DPP-4 inhibitors, often called "gliptins," are oral medications that work on the same hormonal pathway as GLP-1 agonists but in a more subtle way. They block an enzyme called dipeptidyl peptidase-4, which normally breaks down incretin hormones. By inhibiting this enzyme, the medications allow your body's natural GLP-1 to stay active longer.
Why They Are Used
While DPP-4 inhibitors like sitagliptin (Januvia) are not as powerful as GLP-1 injections for weight loss or A1C reduction, they are extremely well-tolerated. They do not cause the nausea often seen with GLP-1s and are weight-neutral. They are an excellent option for older patients or those who prefer a simple, once-daily pill with minimal side effects. They are also safe to use in patients with varying degrees of kidney function, though some may require dose adjustments.
Comparison with GLP-1s
Many patients ask why they would choose a DPP-4 inhibitor over a GLP-1 agonist. The main reasons are ease of use (a small pill versus an injection) and a much lower incidence of gastrointestinal side effects. However, it is important to know that you cannot take both a DPP-4 inhibitor and a GLP-1 agonist at the same time, as they work on the same biological pathway and do not provide additional benefits when combined.
Older Classes: Sulfonylureas and TZDs
While newer drugs often take the spotlight, older classes of medications are still used, particularly when cost is a major factor or when other medications are not tolerated.
Sulfonylureas (Insulin Secretagogues)
Sulfonylureas, such as glipizide and glimepiride, are among the oldest diabetes medications. They work by directly stimulating the beta cells in your pancreas to release more insulin. They are very effective at lowering blood sugar quickly and are very inexpensive, making them a common choice for patients without insurance coverage. However, because they force the pancreas to release insulin regardless of your blood sugar level, they carry a high risk of hypoglycemia (low blood sugar) and often cause modest weight gain. Over time, some evidence suggests they may "wear out" the pancreas's ability to produce insulin.
Thiazolidinediones (TZDs)
Thiazolidinediones, like pioglitazone, are "insulin sensitizers." They work by making your fat, muscle, and liver cells more sensitive to the insulin your body already makes. They provide very durable blood sugar control, meaning they work well for a long time without losing effectiveness. However, they can cause fluid retention (edema) and are generally avoided in patients with heart failure. They have also been associated with an increased risk of bone fractures, particularly in postmenopausal women, and a potential (though debated) risk of bladder cancer with long-term use.
Comparing Medication Classes: A Detailed Look
Choosing between these classes involves balancing efficacy, safety, and personal health history. The following table provides a side-by-side comparison of how these classes stack up against each other in key areas.
| Feature | Metformin | GLP-1 RAs | SGLT2i | DPP-4i | Sulfonylureas | TZDs |
|---|---|---|---|---|---|---|
| A1C Lowering | High | Very High | Intermediate | Intermediate | High | High |
| Hypo Risk | Low | Low | Low | Low | High | Low |
| Weight Change | Neutral/Loss | Loss | Loss | Neutral | Gain | Gain |
| CV Benefit | Potential | Proven | Proven | Neutral | Neutral | Potential |
| Cost | Low | High | High | High | Low | Low |
| Administration | Oral | Injection/Oral | Oral | Oral | Oral | Oral |
Practical Considerations for Patients
Beyond the biological effects, there are several practical aspects to consider when starting a new diabetes medication.
Managing Side Effects
For many, the fear of side effects is a major barrier to starting medication. However, most side effects can be managed. For example, the GI issues with metformin and GLP-1s often resolve within a few weeks as the body adjusts. Staying hydrated is crucial when taking SGLT2 inhibitors to prevent dizziness or kidney strain. If you experience persistent side effects, talk to your pharmacist or doctor rather than simply stopping the medication, as there may be an alternative dose or formulation that works better for you.
Monitoring Your Progress
Starting a medication is not a "set it and forget it" process. You will likely need more frequent blood sugar checks (either through finger sticks or a continuous glucose monitor) when starting a new drug. Your doctor will also check your A1C every three months to see if the medication is doing its job. It is helpful to keep a log of your readings and any symptoms you feel, as this data is invaluable for fine-tuning your treatment plan.
How Doctors Choose Your Treatment
The process of selecting a diabetes medication is increasingly patient-centered. Your doctor will likely consider several factors:
- Comorbidities: Do you have heart disease, heart failure, or kidney disease? If so, SGLT2 inhibitors or GLP-1 agonists are usually prioritized regardless of your A1C level [5].
- Weight Goals: Is weight loss a primary goal? GLP-1s are the most effective for this, followed by SGLT2 inhibitors.
- Hypoglycemia Risk: If you have a job where low blood sugar would be dangerous (like driving or operating heavy machinery), drugs with low hypo risk are preferred.
- Cost and Access: Insurance coverage often dictates which of the newer, more expensive medications are accessible. Your pharmacist can often help find manufacturer coupons or assistance programs to lower these costs.
The Importance of Adherence
No medication works if it isn't taken. Adherence—taking your medication exactly as prescribed—is the single most important factor in preventing diabetes complications. If you find it difficult to remember your doses, consider using a pill organizer, a smartphone app, or switching to a once-weekly injection if appropriate. Open communication with your healthcare team about any barriers you face is key to long-term success.
Bottom Line
There is no "one-size-fits-all" medication for Type 2 Diabetes. While metformin remains the standard starting point, the rise of GLP-1 agonists and SGLT2 inhibitors has provided powerful new tools that protect the heart and kidneys while helping with weight management. The best treatment plan is one that you can consistently follow, fits your lifestyle, and effectively manages your blood sugar while minimizing side effects. Always consult with your healthcare provider or pharmacist before making any changes to your medication regimen.
Sources
- American Diabetes Association. (2024). 9. Pharmacologic Approaches to Glycemic Treatment: Standards of Care in Diabetes—2024. Diabetes Care.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). (2023). Insulin, Medicines, & Other Diabetes Treatments.
- FDA. (2023). FDA Approves New Treatment for Heart Failure.
- PubMed. (2023). Comparative Efficacy of GLP-1 Receptor Agonists and SGLT2 Inhibitors.
- American College of Cardiology (ACC). (2024). 2024 Update on the Management of Type 2 Diabetes in Patients with Cardiovascular Disease.
- Mayo Clinic. (2024). Type 2 Diabetes: Diagnosis and Treatment.
Save up to 80% on this medication
Use a free RxGo discount card at 67,000+ pharmacies — no sign-up, no insurance needed.
About the Author
RxGuide Editorial Team, PharmD, RPh
Clinical Pharmacist & Medical Writer
The RxGuide editorial team is composed of licensed pharmacists and clinical medical writers with expertise in pharmacology, drug safety, and patient education. All clinical content is reviewed against current FDA labeling, peer-reviewed literature, and established clinical guidelines before publication.
Related Articles
Zova Health
Protect the Architecture · GLP-1 Protocol
Don't just lose weight. Preserve your health.
GLP-1 medications can cause up to 39% muscle loss alongside fat. Zova's evidence-based protocol — validated by Lancet Diabetes & Endocrinology 2024 — combines AI-powered leucine tracking, injection-day adaptive nutrition, and progressive resistance training to reduce that to just 8.7%.
No credit card. No commitment. Early access only.
Clinical validation:
Structured protein protocols preserved 78% more lean mass vs. standard GLP-1 use alone. — Lancet Diabetes & Endocrinology, 2024
Get the RxGo app — free prescription discounts on the go
Works at 67,000+ pharmacies · No membership needed