When Senator Bernie Sanders grilled Novo Nordisk CEO Lars Fruergaard Jørgensen before the Senate Health Committee in September 2024, he opened with a single, devastating question: why does the same vial of Ozempic cost $969 a month in the United States, $155 in Canada, $122 in Denmark, and just $59 in Germany?1
Jørgensen did not dispute the numbers. He had no satisfactory answer. And the exchange crystallized a question that tens of millions of American patients, employers, and policymakers have been asking for years: how can the same drug, manufactured by the same company, cost sixteen times more in one wealthy country than in another?
The answer involves no single villain. It is the product of a uniquely American system built over decades — a system that deliberately chose not to regulate drug prices, that allowed patent protections to extend far beyond initial exclusivity periods, and that created a labyrinthine rebate architecture that obscures what anyone actually pays. Understanding why Ozempic costs what it costs in the US requires understanding each of these layers.
The Numbers: A Global Price Comparison
The most rigorous international price comparison for Ozempic comes from the Peterson-KFF Health System Tracker, which in August 2023 published list prices for a one-month supply of Ozempic (semaglutide 1.0mg, four injections) across ten wealthy OECD nations, converted to US dollars at June 2023 exchange rates.2
| Country | Ozempic Monthly List Price (USD) | Ratio vs. US |
|---|---|---|
| United States | $936 | 1.0× (baseline) |
| Japan | $169 | 5.5× cheaper |
| Canada | ~$230 | 4.1× cheaper |
| Sweden | ~$93 | 10.1× cheaper |
| United Kingdom | $93 | 10.1× cheaper |
| Australia | $87 | 10.8× cheaper |
| France | $83 | 11.3× cheaper |
| Germany | $59 | 15.9× cheaper |
Source: Peterson-KFF Health System Tracker, August 2023. Prices are list prices; net prices after rebates may differ.
By the time of the September 2024 Senate hearing, the US list price had risen to $969 per month — a 3.5% increase in just over a year. Novo Nordisk has raised Ozempic's list price every year since its 2018 US launch. By early 2026, the US list price had reached $1,027.51 per month for Ozempic and $1,349 per month for Wegovy, the higher-dose semaglutide approved for weight loss.3
The gap is not unique to Ozempic. A 2024 analysis by the HHS Assistant Secretary for Planning and Evaluation (ASPE) found that US prescription drug prices across all drugs — brands and generics combined — were 2.78 times higher than prices in 33 OECD comparison countries in 2022.4 For brand-name drugs alone, the gap is even wider.
How Other Countries Keep Prices Low
The short answer is that every other wealthy country has a mechanism to say no to a drug company's asking price. The United States, until the Inflation Reduction Act of 2022, had no such mechanism at all.
The UK: Cost-Effectiveness Thresholds
The National Institute for Health and Care Excellence (NICE) in England evaluates every new drug against a cost-effectiveness threshold of approximately £20,000–£30,000 per quality-adjusted life year (QALY). If a drug does not demonstrate sufficient clinical benefit relative to its cost, NICE recommends against coverage on the National Health Service. This gives the NHS enormous negotiating leverage: Novo Nordisk can either accept a lower price or lose access to the entire UK market.
For Ozempic, NICE's assessment of semaglutide for type 2 diabetes concluded it was cost-effective — but only at the price Novo Nordisk agreed to accept, which was $93 per month, less than one-tenth of the US list price.
Germany: The AMNOG Process
Germany uses a system called AMNOG (Arzneimittelmarkt-Neuordnungsgesetz), under which new drugs are launched at the manufacturer's chosen price for exactly one year. During that year, the Federal Joint Committee (G-BA) assesses the drug's "added benefit" compared to existing therapies. The result of that assessment determines the negotiated price for all subsequent years.
For Ozempic, the G-BA found "non-quantifiable added benefit" — meaning the drug works, but the evidence base for its superiority over existing treatments was limited. This assessment gave payers leverage to negotiate aggressively, resulting in the $59 monthly price cited by Senator Sanders. Germany's price is not a subsidy; it is the price Novo Nordisk agreed to in order to remain on the German formulary.
Canada: Reference Pricing with a Ceiling
Canada's Patented Medicine Prices Review Board (PMPRB) historically capped patented drug prices at the median price charged in seven comparator countries: France, Germany, Italy, Sweden, Switzerland, the UK, and the US. The inclusion of the US in that basket — the highest-priced market in the world — has historically inflated Canadian prices relative to European peers. Even so, Canada's price of $155–$230 per month for Ozempic is roughly four to six times lower than the US list price.
Australia: The Pharmaceutical Benefits Scheme
Australia's Pharmaceutical Benefits Scheme (PBS) is a national formulary under which the government negotiates prices directly with manufacturers and then subsidizes approved drugs for all citizens. Drugs that do not meet the PBS's cost-effectiveness criteria are not subsidized, which means patients pay the full price out of pocket — a powerful incentive for manufacturers to negotiate.
France: Centralized HTA and Price Agreements
France's Haute Autorité de Santé (HAS) evaluates drugs for their "medical service rendered" (SMR) and "improvement in medical service rendered" (ASMR). The Economic Committee on Health Products (CEPS) then negotiates prices based on those assessments. Ozempic's French price of $83 per month reflects a negotiated agreement between Novo Nordisk and the French government.
Why the US Is Different
The United States has none of these mechanisms at the federal level — or rather, it did not until 2022. The reasons are structural, political, and historical.
No Federal Price Negotiation (Until the IRA)
For most of Medicare's history, a provision of the 2003 Medicare Modernization Act explicitly prohibited the federal government from negotiating drug prices. This "non-interference clause" was inserted at the behest of the pharmaceutical industry and meant that Medicare — the largest single drug purchaser in the world, covering 67 million Americans — paid whatever price manufacturers chose to set.
The Inflation Reduction Act of 2022 repealed this prohibition and authorized CMS to negotiate prices for a small number of high-cost drugs. The first ten negotiated prices took effect January 1, 2026 — but Ozempic was not among them. Semaglutide products are expected to enter the second negotiation cycle, with negotiated prices potentially taking effect in 2027.5
The PBM Rebate System
One of the most counterintuitive aspects of US drug pricing is that the "list price" — the number that appears on pharmacy receipts and in international comparisons — is not what most payers actually pay. Pharmacy Benefit Managers (PBMs), which administer drug benefits for insurers and employers, negotiate confidential rebates with manufacturers in exchange for favorable formulary placement.
For Ozempic, Novo Nordisk's CEO told the Senate committee that for every dollar the company charges, it gives approximately 74 cents back to PBMs and insurance companies in rebates and fees.1 If accurate, this would imply a net price of roughly $252 per month — still far above the German price of $59, but dramatically lower than the $969 list price.
The rebate system creates a perverse incentive: manufacturers raise list prices specifically to have more room to offer rebates, which PBMs then count as savings. The result is a system that obscures the true cost of drugs, rewards high list prices, and leaves uninsured patients — who pay list price at the pharmacy counter — paying the most of anyone.
Patent Protections and Exclusivity Extensions
Novo Nordisk holds a web of patents on semaglutide that extend well beyond the drug's initial approval. The core semaglutide compound patent expires in 2026, but formulation patents, delivery device patents, and method-of-use patents extend protection on specific products through 2032 and beyond.6
In the US, pharmaceutical companies can file "citizen petitions" with the FDA to delay generic approvals, list additional patents in the Orange Book to trigger automatic 30-month stays, and pursue "product hopping" — making minor changes to a drug to extend exclusivity. These strategies are legal in the US and are used extensively. In Europe, patent law is similar, but health technology assessment bodies can effectively limit a drug's commercial life by refusing to reimburse it at high prices.
The R&D Cost Argument
Novo Nordisk and the pharmaceutical industry broadly argue that high US prices are necessary to fund the research and development of new drugs. The US, they argue, effectively subsidizes drug innovation for the rest of the world by paying premium prices while other countries free-ride on American R&D investment.
There is some truth to this argument. The US does account for a disproportionate share of global pharmaceutical revenue, and that revenue does fund significant R&D. But critics note several problems with the argument as applied to Ozempic specifically.
First, semaglutide's foundational research was conducted at the University of Copenhagen and funded in part by Danish government grants — not by Novo Nordisk alone.7 Second, a 2024 study published by Yale School of Medicine researchers found that Ozempic could be manufactured profitably for $0.89 to $4.73 per month, including a profit margin — implying that the $969 list price represents a markup of 200 to 1,000 times manufacturing cost.8 Third, a March 2026 preprint analysis found that generic injectable semaglutide could be produced for $28 to $140 per person per year ($2.33 to $11.67 per month) once patents expire.9
The Compounding Pharmacy Window — and Its Closure
During the 2022–2025 Ozempic and Wegovy shortage, a legal loophole allowed compounding pharmacies to manufacture copies of semaglutide. Under US law, compounding pharmacies can produce copies of FDA-approved drugs when those drugs appear on the FDA's drug shortage list. At its peak, compounded semaglutide was available from telehealth companies for $150 to $400 per month — a fraction of the brand-name price.
On February 21, 2025, the FDA declared the semaglutide shortage "resolved" and removed semaglutide from the 506e shortage list.10 Compounding pharmacies were given 60 to 90 days to wind down operations. By April 22, 2025, most compounding of semaglutide had ceased. The FDA followed up on February 6, 2026, announcing its intent to take action against non-FDA-approved GLP-1 drugs still on the market.11
The closure of the compounding window returned millions of patients to a stark choice: pay the brand-name list price, find insurance coverage, or go without.
What Patients Actually Pay
The list price is the worst-case scenario. What patients actually pay depends heavily on their insurance status.
With commercial insurance: Most commercially insured patients pay a copay of $25 to $150 per month for Ozempic when it is covered for diabetes. Coverage for Wegovy (weight loss) is more variable; many plans still exclude it. Novo Nordisk offers a savings card that reduces out-of-pocket costs to $25 per month for eligible commercially insured patients.
On Medicare Part D: Before the IRA's $2,000 out-of-pocket cap took effect in 2025, Medicare patients could face thousands of dollars in annual out-of-pocket costs for Ozempic. The IRA's cap now limits total out-of-pocket spending to $2,000 per year for all Part D drugs, providing meaningful relief. Medicare does not yet cover Wegovy for weight loss.
Uninsured: Uninsured patients pay the full list price — $1,027 per month — unless they qualify for Novo Nordisk's NovoCare patient assistance program, which offers Ozempic for $499 per month for uninsured patients with incomes below certain thresholds. For context, the federal poverty level for a single adult in 2025 is $15,060 per year.
With GoodRx: GoodRx coupons reduce Ozempic's price to approximately $850 to $950 per month at major pharmacy chains — a modest discount from list price, but still far above what patients in other countries pay.
The IRA and What Comes Next
The Inflation Reduction Act represents the most significant change to US drug pricing policy in two decades. Beyond the $2,000 out-of-pocket cap, the IRA requires manufacturers to pay rebates to Medicare if they raise prices faster than inflation — a provision that has already slowed Novo Nordisk's US price increases.
Most importantly, the IRA's Medicare negotiation program is expanding. The first ten drugs negotiated for 2026 were dominated by blood thinners, diabetes medications, and cancer drugs. The second cycle, covering drugs for 2027, is expected to include semaglutide products given their enormous Medicare spending impact. A 2024 Senate HELP Committee analysis estimated that if half of all eligible Americans took GLP-1 drugs, the annual cost would exceed $400 billion — making negotiated pricing a fiscal necessity.1
Novo Nordisk has already signaled awareness of the coming negotiation. In 2024, the company announced a voluntary price reduction to $499 per month for uninsured Americans through its NovoCare program — a move widely interpreted as a pre-emptive effort to demonstrate good faith before mandatory negotiation begins.
The Bigger Picture
Ozempic's pricing gap is not an anomaly. It is a window into a system that produces the same outcome across hundreds of drugs. The US pays more for Humira, more for Keytruda, more for Eliquis, more for virtually every major brand-name drug than any other wealthy country. The ASPE analysis found that US brand-name drug prices are, on average, 3.44 times higher than in peer nations.4
The difference is not innovation. It is not manufacturing quality. It is not even, primarily, R&D cost recovery. It is the absence of a mechanism to say no.
Every other wealthy country has built that mechanism — through health technology assessment, reference pricing, national formularies, or direct government negotiation. The US is building one, slowly, through the IRA. Whether it will be enough to close a gap measured in multiples — not percentages — remains to be seen.
For the 8.8 million Americans who will benefit from the first round of Medicare negotiated prices in 2026, the answer matters enormously. For the millions more who take Ozempic and Wegovy and cannot afford them, it matters even more.
Key Takeaways
The core facts of the Ozempic pricing gap can be summarized as follows. The US list price for Ozempic reached $1,027 per month by early 2026, compared to $59 in Germany, $83 in France, $87 in Australia, $93 in the UK, and approximately $155–$230 in Canada. The gap exists because the US is the only wealthy country without a systematic mechanism for government drug price negotiation or health technology assessment at the national level. The PBM rebate system obscures true net prices but does not eliminate the gap; even after rebates, US net prices remain far above international levels. The Inflation Reduction Act of 2022 introduced Medicare drug price negotiation for the first time, with semaglutide products expected to enter the second negotiation cycle for 2027. A Yale study found Ozempic could be manufactured profitably for under $5 per month, and a 2026 analysis found generic semaglutide could cost $28–$140 per year once patents expire — suggesting the current price reflects market power, not production economics.
References
Footnotes
-
Sanders, B. (2024, September 24). Why Is Novo Nordisk Charging Americans with Diabetes and Obesity Outrageously High Prices for Ozempic and Wegovy? Senate HELP Committee hearing. https://www.help.senate.gov/hearings/why-is-novo-nordisk-charging-americans-with-diabetes-and-obesity-outrageously-high-prices-for-ozempic-and-wegovy ↩ ↩2 ↩3
-
Amin, K., Telesford, I., Singh, R., & Cox, C. (2023, August 17). How do prices of drugs for weight loss in the U.S. compare to peer nations' prices? Peterson-KFF Health System Tracker. https://www.healthsystemtracker.org/brief/prices-of-drugs-for-weight-loss-in-the-us-and-peer-nations/ ↩
-
Novo Nordisk. (2026). Ozempic (semaglutide) US list price. Internal pricing data cited in Bloomberg, March 2026. ↩
-
HHS Office of the Assistant Secretary for Planning and Evaluation. (2024, January 31). Comparing Prescription Drug Prices in the United States and Other Countries. https://aspe.hhs.gov/reports/comparing-prescription-drugs ↩ ↩2
-
Centers for Medicare & Medicaid Services. (2024, August 15). Medicare Drug Price Negotiation Program: Negotiated Prices for Initial Price Applicability Year 2026. https://www.cms.gov/newsroom/fact-sheets/medicare-drug-price-negotiation-program-negotiated-prices-initial-price-applicability-year-2026 ↩
-
Levi, J., Cross, S., Ramesh, N., Venter, F., & Hill, A. (2026, March 4). How Low Could Semaglutide Prices Fall? An Analysis of Production Cost and Implications for Global Access Ahead of Patent Expiry. medRxiv. https://www.medrxiv.org/content/10.64898/2026.03.04.26347508v1 ↩
-
Knudsen, L.B., & Lau, J. (2019). The Discovery and Development of Liraglutide and Semaglutide. Frontiers in Endocrinology, 10, 155. https://doi.org/10.3389/fendo.2019.00155 ↩
-
Gotham, D., et al. (2024, March). Estimated minimum costs of production for GLP-1 receptor agonists. Yale School of Medicine / BMJ Global Health. Reported by CNBC, March 27, 2024. https://www.cnbc.com/2024/03/27/novo-nordisk-ozempic-can-be-made-for-less-than-5-a-month-study.html ↩
-
U.S. Food and Drug Administration. (2025, February 21). FDA clarifies policies for compounders as national GLP-1 supply begins to stabilize. https://www.fda.gov/drugs/drug-safety-and-availability/fda-clarifies-policies-compounders-national-glp-1-supply-begins-stabilize ↩
-
U.S. Food and Drug Administration. (2026, February 6). FDA Intends to Take Action Against Non-FDA-Approved GLP-1 Drugs. https://www.fda.gov/news-events/press-announcements/fda-intends-take-action-against-non-fda-approved-glp-1-drugs ↩
Save up to 80% on this medication
Use a free RxGo discount card at 67,000+ pharmacies — no sign-up, no insurance needed.
Related Articles
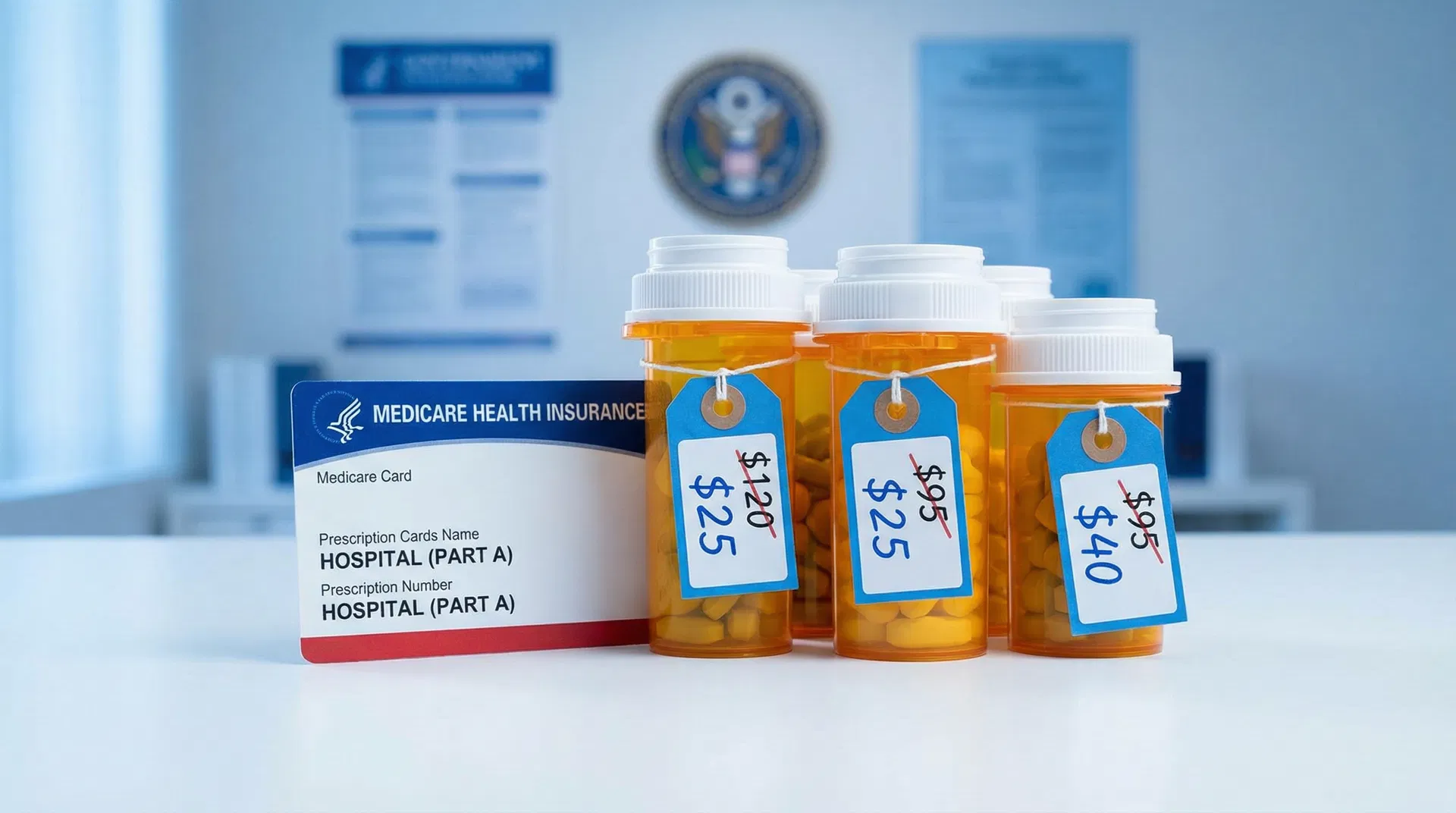
The 10 Drugs Medicare Negotiated and What They'll Cost in 2026
For the first time in Medicare's 60-year history, the federal government negotiated drug prices directly with pharmaceutical manufacturers. On January 1, 2026, those negotiated prices went into effect for 8.8 million Medicare patients. Here is the complete price table, the savings data, and what comes next.

How Much Does a Generic Save? A Data Analysis Across 26 Drug Classes
Generic drugs save Americans an estimated $400 billion per year, but the savings vary dramatically by drug class. Our original analysis of pricing data across 26 drug classes reveals which classes offer the greatest generic savings — and which have no generic options at all.
GLP-1 Drug Spending Rose 500% in 5 Years — What It Means for Patients
Total US spending on GLP-1 drugs like Ozempic and Wegovy surged from $13.7 billion in 2018 to $71.7 billion in 2023 — a 500% increase. We analyze the data behind the fastest-growing drug category in American history and what it means for affordability.
Zova Health
Protect the Architecture · GLP-1 Protocol
Don't just lose weight. Preserve your health.
GLP-1 medications can cause up to 39% muscle loss alongside fat. Zova's evidence-based protocol — validated by Lancet Diabetes & Endocrinology 2024 — combines AI-powered leucine tracking, injection-day adaptive nutrition, and progressive resistance training to reduce that to just 8.7%.
No credit card. No commitment. Early access only.
Clinical validation:
Structured protein protocols preserved 78% more lean mass vs. standard GLP-1 use alone. — Lancet Diabetes & Endocrinology, 2024
Get the RxGo app — free prescription discounts on the go
Works at 67,000+ pharmacies · No membership needed
